There is increased awareness in gut health related to a variety of GI issues such as IBS, Colitis, Crohn’s and small intestinal bacterial overgrowth (SIBO).
Although we have 50 years of literature on SIBO, attention has increased over the last 10 years. People are more aware of SIBO as a diagnosis for chronic, often dismissed functional digestive complaints. Consequently, there is no typical presentation for SIBO. It can be asymptomatic or often mimic other disease states. In general IBS and SIBO are underdiagnosed and therefore, an accurate occurrence rate is unknown. The complaints of SIBO seems to be more common as people age, which may be due to the decrease in natural defenses.
The clinician should suspect SIBO in a client who has a malabsorption syndrome or who has one of the predisposing conditions or presents with IBS-type symptoms.
SIBO is diagnosed clinically by: (1) jejunal aspirate, (2) breath testing and (3) response to treatment with antibiotics.
Combining two of these methods offers the best approach. The breath test is the most common and widely used test to determine if SIBO is present.
SIBO Symptoms:
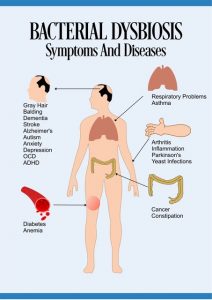 Digestive Tract
Digestive Tract
• Abdominal bloating (gas)
• Belching/flatulence
• Abdominal pain
• Abdominal cramping
• Change in bowel movements: constipation, diarrhea or both
• Nausea
• Heartburn (reflux or GERD)
• Steatorrhea (fat in stool)
• Nutritional deficiencies: B12, iron
Outside of Digestive Tract
• Fatigue
• Weight loss
• Headache
• Joint pain
• Skin issues: rashes, eczema
• Mood symptoms
• Brain fog
Reducing Overgrowth
The classical treatment of SIBO is the use of antibiotic pharmaceuticals. The most recent reviews indicate rifaximin as the safest and most effective. It is a locally absorbed antibiotic and therefore has less occurrence of systemic effects, although it still can disrupt the gastrointestinal microbiota.
If there is both hydrogen and methane gas present, then a second antibiotic has been shown to be more effective.
Dietary Approaches
One dietary therapy to reduce bacterial levels is to follow a liquid elemental diet for 2-3 weeks. This provides all the essential nutrients and amino acids to the gut but is absorbed within the first few feet of the intestine, essentially starving the fermenting bacteria in the small intestine. Clinical success is seen with this method but is on a case-by-case basis. In addition, people who are already low in weight or have blood sugar stability issues must be careful.
After the bacteria have been reduced, a repeat breath test or symptom evaluation will determine how successful the treatment has been. If symptoms are 90% better, the next step will be prevention of recurrent SIBO. If symptoms are still present after the appropriate time on antimicrobials, a repeat breath test may be helpful to determine how much the levels have changed and that will influence the prognosis and length of treatment.
There is no diet that is 100% effective at managing symptoms of SIBO and diet needs to be tailored to the individual. Low-carbohydrate diets commonly used for SIBO include Specific Carbohydrate Diet (SCD), SIBO Specific Diet (by Dr. Siebecker), Low FODMAP, GAPS, Cedar Sinai and Fast Tract Diet. However, none of these diets have been studied for effectiveness with SIBO. These diets are all low carbohydrate and should be used with caution in people at low weight.
Enhancing Motility
The migrating motor complex (MMC) is the movement of the small intestine, which sweeps bacteria through and prevents buildup of bacteria.
The MMC is active during fasting states and is stopped by feedings. Encouraging meal spacing is recommended to allow this system “detoxifies“ the intestine.
Dysregulation of MMC has been implicated in the overgrowth of bacteria in the small intestine. Therefore, fasting and spacing is beneficial.
Ginger, which has prokinetic qualities, can also help reduce some of the uncomfortable symptoms of SIBO.
When SIBO is present, it is thought this disrupts the lining of the small intestine, which then minimizes absorption of certain nutrients. After the bacterial overgrowth has been resolved, the small intestinal lining should heal itself. However, additional support with glutamine can be helpful.
Stress and Adrenal Balance
Important to reduce stress and address adrenal imbalance as SIBO can take a toll on the body both physically and emotionally. Therefore stress management and lifestyle changes are useful.
Water Quality Is a Significant Source of Exposure
The rationale for including water in the discussion is not that hydration is a new concept; it’s that water quality is not often addressed and is a significant source of toxicant exposure. With access to purified water, you can now encourage your patients to maximize their hydration (at least 1/2 to 3/4 their body weight in ounces) as it is essential to flushing out waste not only at the cellular level but in supporting the GI tract and kidneys as they flush out toxins.
For more information on filtration:
http://www.ewg.org/tap-water/whats-in-yourwater.php
Healing the Gut
The benefits of Healthy Microbiome/ Gut Flora:
Digestion of Food, Synthesis of B Vitamins, and Vitamin K, Produce ATP (energy), Inhibit Intestinal Pathogens, Deconjugate Bile Acids. In addition, further benefits of healthy microbiome contribute to enhance Lactose Tolerance and Glucose Balance, Stimulate Immune Function, Maintain Mucosal Integrity, and Metabolize Xenobiotics
Healing the Digestive Tract is Central to Preparing for an Effective Detox.
When the digestive tract is overburdened by inflammatory foods, pathogenic microbes, chronic stress, medications and the wide array of chemicals in processed foods, the gut walls become permeable. Undesirable substances then enter the bloodstream, to be transported to the liver for processing, aka detoxification. The goal in preparing the gut for detox is to decrease the daily burden on the liver so a deeper level of detoxification can be achieved.
Identify Which Diet and Foods Work Well for Your Individual Needs
The starting point for your patient to eliminate the most common inflammatory foods (gluten, dairy, soy, corn and sugar) is essential to improving digestive health and reducing the burden on the liver. Food sensitivity testing is often the easiest path to discerning which foods are creating the most inflammation and to optimize patient compliance, as they are more likely to adhere to a dietary protocol when they see exactly how their immune system reacts to different foods through testing.
Food sensitivity testing is often the easiest path to discerning which foods are creating the most inflammation and optimizing patient compliance, as they are more likely adhere to a dietary protocol when they see exactly how their immune system reacts to different foods.
Decreasing Exposures on How to Reduce Toxicants from Food.
An easy place to start is to avoid the “Dirty Dozen” foods (found on www.ewg.org; there is also a free smartphone app) and only eat organic, free-range animal products. A simple way to reduce some of these exposures is to eat seafood and to lower or eliminate exposure to farmed and high mercury-content fish. Polychlorinated bisphenyls / PCBs (ubiquitous and highly elevated in farmed salmon), with a half-life in the blood of 10-15 years, are associated with breast cancer 1, ADHD 2, diabetes 3 and myocardial infarction. 4 Mercury (found in tuna and other large fish) can bioaccumulate in your tissues with a half-life ranging from 10-50 years!
** the Environmental Working Group (EWG)’s online Consumer Guide to Seafood
Conventional Personal Care Products.
* toxicants with phthalates, Parabens to name a few, can be harmful causing liver toxicatism, and possibly cancer.
Balance the digestive Gut flora.
There are tests that can reveal the state of the gut flora. This laboratory testing helps identify the specific culprits.
*The Indican test is a urine test that gives a simple screening tool for generalized dysbiosis.
*Breath testing is also available to help identify small intestinal bacterial overgrowth/ SIBO.
*Blood testing that measures LPS IgM, IgG and IgA antibodies levels, which are elevated in dysbiosis.
*There are also a variety of stool tests available that not only test for pathogenic or opportunistic overgrowths of bacteria, yeast, and parasites but also show some functional testing of pancreatic function, absorption and inflammation..
Protocols with functional treatments depend on many factors. However, an overall approach is to restore gut function through diet and supplements for the GI tract.
